When we talk about breast cancer, the normal assumption is that we are talking about women getting the disease. But, men can get breast cancer too.
Breast cancer in men usually presents as a painless lump in the breast. Men, however, tend to present with larger cancers and with more advanced disease. In principle, breast cancer in men is treated the same way as breast cancer in women, but there are some minor differences. Let’s look in more detail on the risk factors, treatment options and outcomes.
What does breast cancer in men look like?
As mentioned earlier, breast cancer in men normally presents as a painless lump, usually behind the nipple area, although it can also occur anywhere in the breast. It can also present with nipple retraction, skin changes and nipple discharge. So, the symptoms are similar to those in women.
Men can also have a condition called gynaecomastia, a benign condition that also usually presents as a lump behind the nipple area. Clinical examination and imaging should be able to differentiate between these two conditions. If the appearance is suspicious, then we will perform a biopsy to confirm the exact nature of the lump
Breast cancer in men – statistics
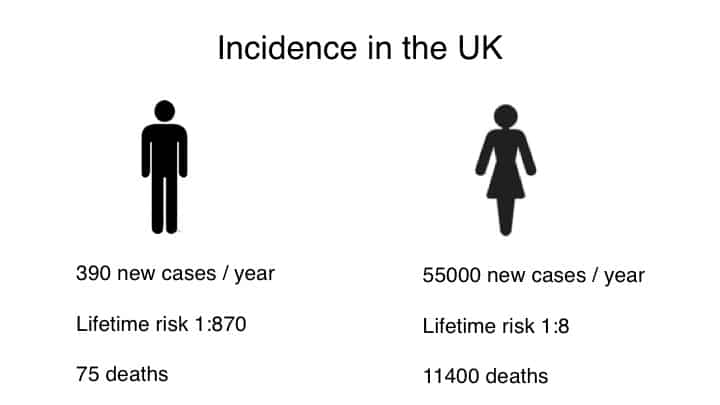
Male breast cancer represents less than 1% of all cancers in men, and less than 1% of breast cancers. In the UK, we see roughly 390 new cases per year, with a lifetime risk of 1:870. Compare this to 55,000 new cases of female breast cancer per year in the UK, with a lifetime risk of 1 in 8, the incidence is comparatively low.
What are the risk factors of breast cancer in men?
1. Increasing age.
Like most cancers, the risk of breast cancer in men increases with age. The incidence steadily increases with age, peaking at 72 yrs with an average age of 67 yrs compared to 62 yrs for women. So age is a risk factor and we know that men with breast cancer do present at an older age.
2. Ethnicity
The risk of breast cancer in black men is greater than white men. Black men also have poorer prognostic features such as larger tumours, axillary lymph node positivity and higher grade tumours compared to white men.
3. Family history
Family History plays an important role in development of breast cancer in men. If a man has a sister who has breast cancer, this has a more significant impact compared to if only his mother had breast cancer.
The risk of breast cancer, however, increases 10 fold if both mother and a sister have breast cancer.
4. Gene mutation
If you are a man and have a BRCA 2 gene mutation, then you have an increased risk of breast cancer with a lifetime risk of about 5-10% compared to the general population risk of 0.1%. ASCO (American Society of Clinical Oncology) has recommended genetic counselling and testing to all men with breast cancer. The association of male breast cancer with a BRCA 1 gene mutation is less strong with a risk of 1%.
5. Radiation
The most robust evidence we have showing how high radiation exposure increases male breast cancer risk is from looking at survivors of the Japanese atomic bomb survivors.
Chest wall irradiation such as in the case for lymphoma may also increase the risk of male breast cancer.
6. Kleinfelter’s syndrome
A high oestrogen level or low testosterone level increases the risk of developing breast cancer in men. Kleinfelter’s syndrome is a genetic order where males are born with an extra X chromosome (it is is also known as the XXY syndrome). It occurs at about 1:1000 live births.
Affected men typically have under-developed testis that does not produce as much testosterone as usual. There is an increased risk of breast cancer in men with this syndrome.
7. Liver disease and obesity
Data from case-control studies suggest that increases in oestradiol levels are associated with male breast cancer. Examples of this include condition such as in liver cirrhosis or when there is exogenous oestrogen use.
Men with a BMI (body mass index) of >30 has an 80% increased risk compared with men with a BMI of <25.
How do we investigate breast lumps in men?
Like for any breast lump, you will need to see a breast specialist in a breast clinic. We will examine the breast including the lump during a physical examination. Using an ultrasound machine, we will scan the lump that will help us decide what it may be.
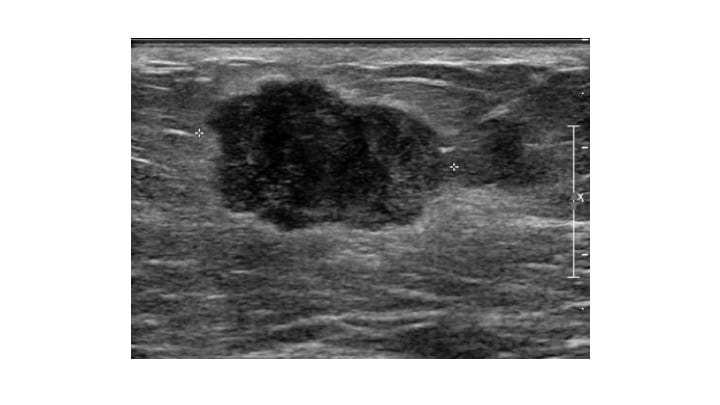
In some clinics, you may also get a mammogram. Non-cancerous lumps (benign lumps) have characteristic features, both when examined and on imaging. If it looks benign, then no further investigations are needed. However, if it is suspicious, then a biopsy will be performed.
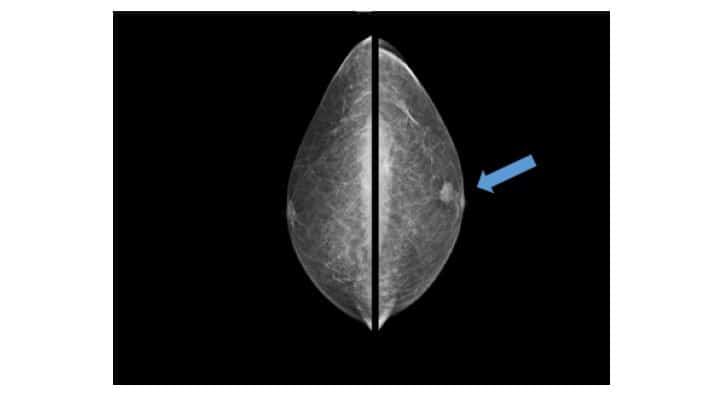
Because there is a lack of screening programmes and awareness, breast cancer in men usually presents as larger cancers compared to women. We also find that lymph node metastases, as a result, is more common (42% of males compared to 33% of women
Do you see the same type of breast cancer in men as you do in women?
Yes, we do. Male breast cancer commonly originates from the ductal system and so you commonly see ductal carcinomas. The male breasts consist of very few lobules, and so lobular cancers are less common.
Overall, male breast cancer is more likely to be oestrogen receptor-positive and Her2 negative. They are less likely to be triple-negative (i.e ER negative, PR negative, Her2 negative).
How do you treat it?
You treat it in a similar fashion to female breast cancers. Depending on the individual, this may involve surgery, chemotherapy, radiotherapy and endocrine treatment (tablets).
1. Surgery
Traditionally, a mastectomy i.e. removal of the entire breast would be the surgery most commonly recommended. Because the male breast does not contain much breast tissue, a mastectomy ensures complete removal of the cancer. By doing this, we also make sure that we achieve a good cosmetic outcome.
However, if the lump is small and there is a considerable amount of breast tissue , then we can perform a lumpectomy. It is important to make sure however that there is enough breast tissue available in order to allow closure of the defect.
2. Radiotherapy
Observational studies have shown that breast conservation with radiotherapy has similar survival rates compared to those who have had a mastectomy, and yet we don’t do enough breast conservation surgery in men. The data suggests that roughly only 52% of men with breast cancer who have had breast conservation surgery will get radiotherapy.
3. Chemotherapy
Like in women, men who are eligible should be offered chemotherapy both in the neoadjuvant and adjuvant setting. Although the data on the benefits of chemotherapy in men is from observational studies, it has been shown to improve survival rates.
4. Endocrine treatment
Since most male breast cancers are oestrogen positive, endocrine treatment plays an important role in treatment. Tamoxifen is the most studied and is the recommended treatment.
Studies have noted survival among men with breast cancer are improved with using adjuvant tamoxifen, but not with an aromatase inhibitor. We think the reason for this is the inability of an aromatase inhibitor to fully suppress the level of circulating oestrogen in men. Thus, an aromatase inhibitor cannot be recommended without an LHRH agonist such as Zoladex.
Is there a survival difference between men and women with breast cancer?
The American SEER (Surveillance Epidemiology and End Results registry) database has shown that men have poorer survival for stages I-III compared to women. However, the relative survival rates obtained after adjusting for older age at diagnosis and poorer life expectancy shows survival rates are quite similar between men and women.
Summary
Male breast cancer is not common but does exist. I think it is important to increase awareness to encourage men to do a self-examination, enabling them to seek medical attention early.
Most studies in breast cancer are on women, and the majority of treatment decisions for men are based on these studies. We, therefore, need more studies that look into breast cancer in men specifically. The Male Breast Cancer Study is an example of a study that is looking into the genetic, environmental and lifestyle factors that may contribute to the development of breast cancer in men.
Featured image by Photo by Aaron Andrew Ang on Unsplash


